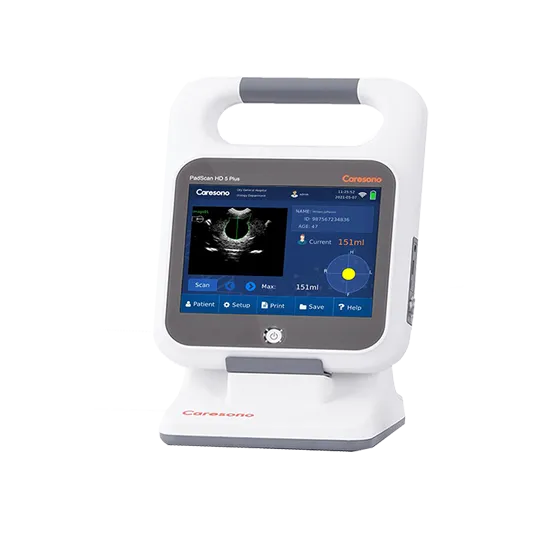
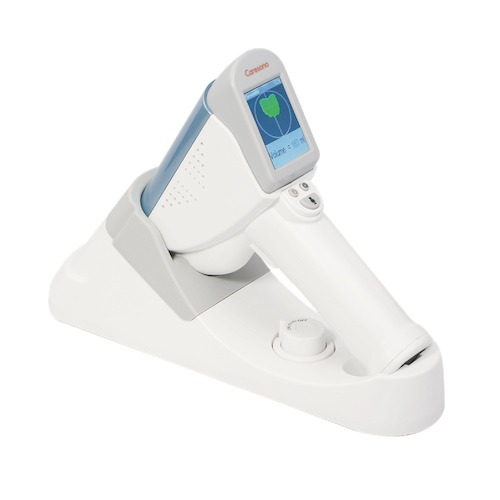
How Bladder Scanners Help with Urinary Retention: Clinical Benefits and Applications
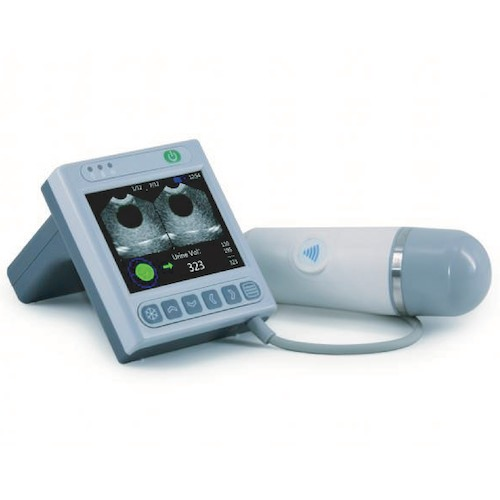
How Bladder Scanners Help with Urinary Retention: Clinical Benefits and Applications
Urinary retention represents a significant clinical challenge affecting millions of patients across diverse healthcare settings. This comprehensive examination explores how bladder scanners provide non-invasive assessment of urinary retention, improve patient outcomes, reduce complications, and enhance clinical decision-making.
Understanding Urinary Retention
Urinary retention is the inability to completely empty the bladder. It can be acute (sudden onset) or chronic (developing gradually over time), and it affects patients across all age groups, though it is particularly common in elderly populations and those with certain medical conditions.
Types of Urinary Retention
Acute urinary retention presents as a sudden inability to void despite a full bladder, often accompanied by significant pain and discomfort. This medical emergency requires prompt intervention to relieve bladder distension and prevent complications.
Chronic urinary retention develops gradually, with patients retaining increasing amounts of urine after voiding. Many patients with chronic retention are unaware of the problem, as the bladder gradually accommodates larger volumes without causing acute symptoms. This silent progression can lead to serious complications if undetected.
Causes and Risk Factors
Urinary retention results from various underlying conditions:
Bladder outlet obstruction is the most common cause, particularly in men with benign prostatic hyperplasia (BPH). The enlarged prostate compresses the urethra, impeding urine flow and eventually leading to incomplete bladder emptying.
Neurogenic bladder dysfunction occurs when nerve damage affects bladder control. Conditions such as diabetes, multiple sclerosis, spinal cord injury, and stroke can disrupt the neural pathways controlling bladder function, resulting in retention.
Medications can contribute to urinary retention through various mechanisms. Anticholinergics, antihistamines, decongestants, and opioids can all impair bladder contractility or increase outlet resistance.
Post-operative retention is common following surgery, particularly procedures involving anesthesia, pelvic surgery, or orthopedic operations. Multiple factors contribute, including anesthetic effects, pain, immobility, and fluid management.
Detrusor underactivity involves weakened bladder muscle contractility, reducing the bladder's ability to generate sufficient pressure for complete emptying. This condition becomes more common with aging.
The Critical Role of Bladder Scanners in Retention Assessment
Bladder scanners have revolutionized urinary retention assessment by providing quick, accurate, non-invasive measurement of bladder volume. This technology enables clinicians to detect retention early, guide intervention decisions, and monitor treatment effectiveness without the risks and discomfort of catheterization.
Non-Invasive Volume Measurement
The fundamental advantage of bladder scanning is non-invasive assessment. Traditional methods of determining bladder volume required catheterization, which carries risks of infection, urethral trauma, and patient discomfort. Bladder scanners use ultrasound technology to visualize the bladder and calculate volume without any invasive procedures.
This non-invasive approach is particularly valuable for screening and monitoring applications where repeated assessments are necessary. Patients can undergo multiple bladder scans throughout the day without cumulative risk, enabling comprehensive evaluation of bladder function patterns.
Rapid Point-of-Care Assessment
Bladder scanners provide immediate results at the point of care, eliminating delays associated with traditional assessment methods. Within seconds, clinicians can determine bladder volume and make informed decisions about intervention timing.
This rapid assessment capability is crucial in acute care settings where timely intervention prevents complications. Emergency department staff can quickly identify acute retention and initiate appropriate treatment. In post-operative settings, nurses can monitor bladder function and intervene before retention becomes severe.
Objective Measurement for Clinical Decision-Making
Bladder scanners provide objective, quantifiable data that removes guesswork from retention assessment. Rather than relying on subjective symptoms or physical examination findings, clinicians have precise volume measurements to guide decisions.
Post-void residual (PVR) measurement is particularly valuable. By scanning immediately after the patient voids, clinicians can determine how much urine remains in the bladder. Elevated PVR indicates incomplete emptying and guides further evaluation and treatment.
Clinical Applications of Bladder Scanning in Retention Management
Emergency Department Assessment
Acute urinary retention commonly presents to emergency departments, requiring rapid assessment and intervention. Bladder scanners enable immediate confirmation of retention and volume measurement, guiding treatment decisions.
Differentiating acute retention from other causes of lower abdominal pain is straightforward with bladder scanning. A distended bladder on ultrasound confirms retention, while a collapsed bladder suggests alternative diagnoses.
Volume-guided catheterization decisions optimize patient care. Moderate bladder volumes may respond to conservative measures, while large volumes require immediate catheterization. Knowing the volume helps clinicians counsel patients about expected relief and potential complications.
Post-Operative Monitoring
Post-operative urinary retention (POUR) affects 5-70% of surgical patients depending on the procedure type, anesthesia, and patient factors. Bladder scanning enables systematic post-operative monitoring to detect retention early.
Protocol-driven scanning at specified intervals (e.g., every 4-6 hours) identifies retention before symptoms become severe. Many patients, particularly those receiving pain medications, may not recognize bladder fullness until retention is advanced.
Intervention thresholds based on bladder volume guide catheterization decisions. Common thresholds include 400-600ml, though specific values may vary based on institutional protocols and patient factors.
Avoiding unnecessary catheterization is equally important. Patients with normal bladder volumes do not require catheterization, reducing infection risk and improving patient experience.
Chronic Retention Management in Primary Care
Primary care providers increasingly use bladder scanning to evaluate lower urinary tract symptoms and detect chronic retention. Many patients with chronic retention present with vague symptoms or are entirely asymptomatic.
Screening high-risk patients identifies retention before complications develop. Men over 50 with BPH symptoms, diabetic patients with neuropathy, and patients on anticholinergic medications benefit from periodic bladder scanning.
Post-void residual measurement during office visits provides objective assessment of bladder emptying efficiency. Elevated PVR (typically >200ml) indicates retention requiring further evaluation and treatment.
Monitoring treatment effectiveness is streamlined with bladder scanning. Patients started on medications for BPH or overactive bladder can have PVR measured at follow-up visits to assess therapeutic response objectively.
Long-Term Care and Geriatric Settings
Elderly residents in care facilities have high rates of urinary retention due to multiple risk factors including medications, mobility limitations, cognitive impairment, and age-related bladder changes. Bladder scanning supports proactive retention management in these settings.
Regular screening of at-risk residents identifies retention early. Residents with declining mobility, new medications, or changes in voiding patterns benefit from bladder volume assessment.
Catheter management decisions are informed by bladder scanning. Residents with indwelling catheters can have bladder volume checked to verify catheter patency. Those being considered for catheter removal can have post-removal PVR measured to assess bladder function.
Reducing unnecessary catheterization improves quality of life and reduces infection risk. Bladder scanning enables staff to distinguish between retention requiring catheterization and other causes of urinary symptoms.
Neurogenic Bladder Management
Patients with neurogenic bladder due to spinal cord injury, multiple sclerosis, or other neurological conditions require ongoing bladder management to prevent complications. Bladder scanning plays a central role in their care.
Intermittent catheterization schedules are optimized using bladder volume data. Rather than catheterizing on a fixed schedule, patients can perform bladder scans to determine when catheterization is needed, improving quality of life while maintaining bladder health.
Monitoring for complications such as autonomic dysreflexia in spinal cord injury patients is enhanced by bladder scanning. Unexpected bladder distension can trigger this dangerous condition, and regular scanning helps prevent it.
Evaluating treatment interventions including medications, botulinum toxin injections, and surgical procedures is facilitated by objective bladder volume measurement before and after treatment.
Clinical Benefits of Bladder Scanning for Retention
Reduced Catheterization Rates
The most significant benefit of bladder scanning is reduced unnecessary catheterization. By providing objective volume data, bladder scanners prevent catheterization in patients with normal or minimally elevated bladder volumes.
Lower catheter-associated urinary tract infection (CAUTI) rates result from reduced catheterization. CAUTIs represent a major source of healthcare-associated infections, increasing morbidity, mortality, and healthcare costs. Each avoided catheterization reduces infection risk.
Decreased urethral trauma is another benefit. Catheterization carries risks of urethral injury, particularly in patients with anatomical abnormalities or when performed by inexperienced operators. Non-invasive bladder scanning eliminates this risk for assessment purposes.
Early Detection and Intervention
Bladder scanning enables early detection of retention before complications develop. Chronic retention often progresses silently, and by the time symptoms appear, bladder function may be significantly compromised.
Preventing bladder overdistension protects bladder function. Severe overdistension can damage bladder muscle, leading to permanent impairment of contractility. Regular bladder scanning in at-risk patients identifies retention at earlier, more reversible stages.
Avoiding renal complications is critical. Chronic retention with high bladder pressures can cause hydronephrosis and renal dysfunction. Early detection and treatment prevent these serious complications.
Improved Patient Comfort and Satisfaction
Non-invasive assessment is far more comfortable than catheterization. Patients appreciate the quick, painless nature of bladder scanning, improving their healthcare experience and satisfaction.
Reduced anxiety accompanies non-invasive procedures. Many patients, particularly those with previous negative catheterization experiences, feel significant anxiety about bladder assessment. Bladder scanning eliminates this source of distress.
Faster symptom relief results from rapid assessment and intervention. Patients with acute retention receive prompt treatment based on immediate bladder volume data rather than waiting for traditional assessment methods.
Enhanced Clinical Efficiency
Bladder scanning improves clinical workflow efficiency. Nurses and physicians can quickly assess bladder volume at the bedside without delays for radiology studies or specialist consultation.
Reduced nursing time for bladder management is significant. Rather than performing catheterization for assessment purposes, nurses can complete bladder scans in seconds, freeing time for other patient care activities.
Decreased healthcare costs result from multiple factors: fewer catheterizations, reduced CAUTIs, prevented complications, and avoided emergency department visits. The cost savings typically justify bladder scanner investment within the first year of use.
Objective Documentation and Quality Improvement
Bladder scanners provide quantifiable, documentable data for medical records. Precise volume measurements support clinical decision-making and provide objective evidence for interventions.
Quality improvement initiatives benefit from bladder scanning data. Healthcare facilities can track catheterization rates, CAUTI incidence, and retention detection rates, using this information to improve protocols and outcomes.
Regulatory compliance is supported by documented bladder assessment. Quality measures increasingly focus on appropriate catheter use and CAUTI prevention, and bladder scanning data demonstrates compliance with best practices.
Best Practices for Bladder Scanning in Retention Assessment
Proper Scanning Technique
Accurate bladder volume measurement requires proper technique. The patient should be positioned supine or semi-recumbent, and the probe should be placed on the lower abdomen above the pubic symphysis, aimed toward the bladder.
Multiple measurements improve accuracy. Performing 2-3 scans and averaging the results reduces measurement variability. Most modern bladder scanners automatically perform multiple measurements and calculate the average.
Optimal timing for post-void residual measurement is within 10-15 minutes after voiding. Longer delays allow continued urine production, potentially overestimating residual volume.
Interpreting Results
Normal bladder volumes vary depending on timing. Pre-void volumes typically range from 300-500ml when patients first feel the urge to void. Post-void residual volumes below 50ml are generally considered normal, though values up to 100ml may be acceptable in elderly patients.
Abnormal findings requiring intervention include:
- Acute retention: volumes >400-600ml with inability to void
- Chronic retention: post-void residual >200ml
- Bladder overdistension: volumes >800-1000ml
Clinical context is essential for interpretation. Bladder volume must be considered alongside symptoms, physical examination findings, and patient history to guide appropriate management.
Integration into Clinical Protocols
Standardized protocols optimize bladder scanning utilization. Facilities should develop clear guidelines for when to perform bladder scans, interpretation of results, and intervention thresholds.
Staff training ensures consistent, accurate technique. All staff members who will perform bladder scanning should receive hands-on training and demonstrate competency before independent use.
Documentation standards should specify what information to record, including bladder volume, timing relative to voiding, patient position, and any interventions performed based on results.
Choosing the Right Bladder Scanner for Retention Assessment
Essential Features
Bladder scanners for retention assessment should provide accurate volume measurement in the clinically relevant range (0-999ml). Accuracy within ±15% or ±15ml meets clinical standards.
Ease of use is critical, particularly in settings where multiple staff members will use the device. Intuitive interfaces and clear displays reduce training requirements and operational errors.
Portability enables point-of-care assessment. Lightweight, handheld designs allow clinicians to bring the scanner to the patient rather than transporting patients to equipment.
Recommended Models
The HD2 Handheld Bladder Scanner offers excellent value for retention assessment with its accurate measurements, long battery life, and affordable price point. Its Expert and Easy modes accommodate varying user skill levels.
The HD5 Plus Wireless Bladder Scanner provides premium features including wireless operation and no-calibration technology, ideal for high-volume clinical settings requiring maximum efficiency.
For budget-conscious facilities, ex-demo models like the Ex-Demo HD2 at £2,650 provide the same functionality as new equipment at significantly reduced cost, making retention assessment accessible to more healthcare settings.
Conclusion
Bladder scanners have transformed urinary retention assessment and management by providing non-invasive, rapid, accurate bladder volume measurement. The clinical benefits are substantial: reduced catheterization rates, lower infection risk, early detection of retention, improved patient comfort, and enhanced clinical efficiency.
From emergency departments managing acute retention to primary care offices screening for chronic retention, from post-operative units monitoring surgical patients to care facilities managing elderly residents, bladder scanners enable better care across all settings where urinary retention occurs.
As an independent supplier with over 15 years of experience, we help UK healthcare providers select bladder scanning equipment optimized for retention assessment. Whether you need premium wireless technology for a busy urology practice or cost-effective ex-demo equipment for a care facility, we provide expert guidance and quality-assured devices to support excellent patient outcomes.
The investment in bladder scanning technology delivers returns through improved patient care, reduced complications, and decreased healthcare costs—making it an essential tool for any facility managing patients at risk for urinary retention.